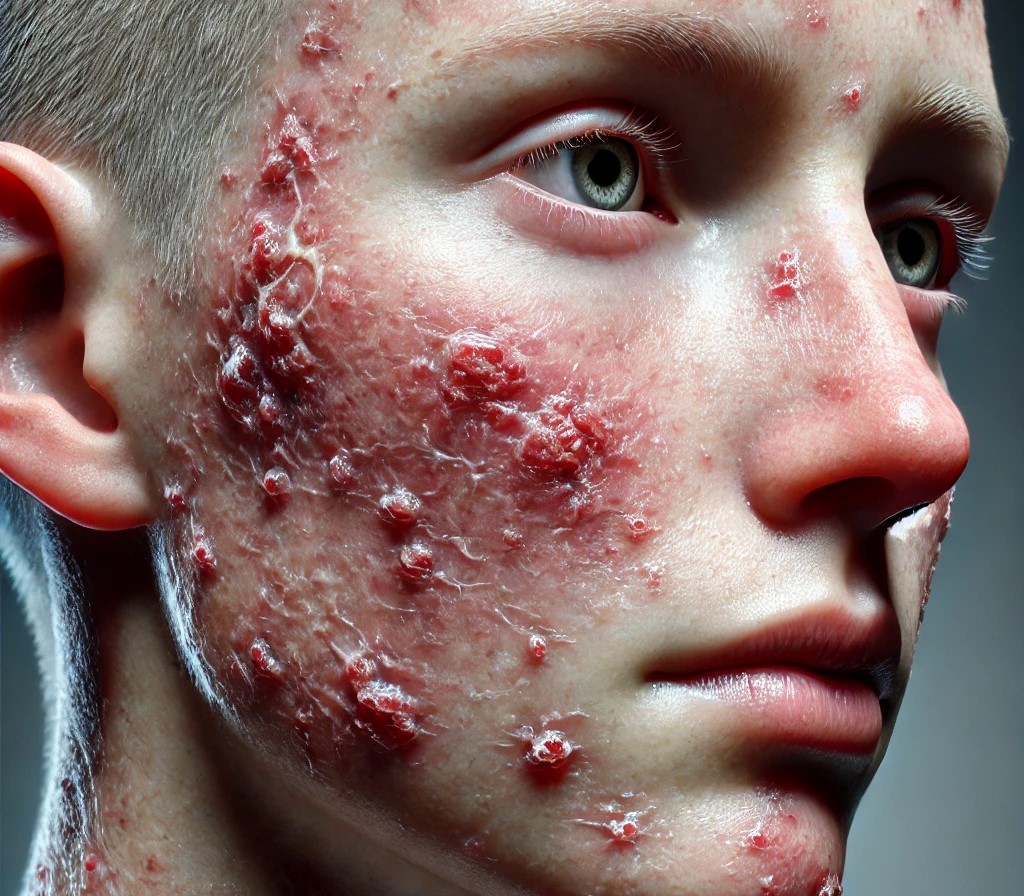
Treating Steroid-Induced Rosacea and Eczema
Steroid-induced rosacea and eczema are skin conditions that arise primarily due to the prolonged use of topical corticosteroids. Both conditions manifest through specific symptoms influenced by unique physiological pathways.
Pathophysiology of Steroid-Induced Skin Conditions
The pathophysiology of steroid-induced skin conditions involves several intricate processes. Prolonged usage of corticosteroids can lead to altered immune responses and thinning of the skin barrier. In rosacea, this may cause increased blood flow or erythema and vessel dilation. For eczema, impaired skin healing further exacerbates the inflammatory response, resulting in scaly, red patches. Genetic susceptibility also plays a crucial role, as certain individuals may be more prone to these effects.
Identifying Symptoms and Variations
Recognizing the symptoms of these skin conditions is essential. Steroid-induced rosacea typically presents with redness, pustule formation, and telangiectasia on the face. Eczema is characterized by itchy, inflamed patches that may become cracked or weepy. Variations exist due to factors such as skin type and duration of steroid use. Monitoring these symptoms helps in differentiating between the two conditions and applying the correct management strategy.
Factors Contributing to Onset and Severity
The onset and severity of steroid-induced rosacea and eczema are influenced by several factors. These include the potency and duration of corticosteroid use, as well as individual genetic factors. Environmental triggers like harsh weather or allergens can exacerbate symptoms. Furthermore, frequent application of topical steroids without professional guidance increases the risk of developing these conditions, emphasizing the importance of careful management.
Treating and Managing Steroid-Induced Skin Conditions
Treating steroid-induced skin conditions involves using alternative topical treatments, systemic medications, and adopting effective lifestyle strategies to manage symptoms and promote skin health.
Topical Treatments and Alternatives
For managing steroid-induced skin conditions, it's important to explore topical treatments that minimize reliance on steroids. Topical calcineurin inhibitors like tacrolimus and pimecrolimus offer an effective alternative due to their immunosuppressive properties without the adverse effects of steroids.
Formulations such as creams, ointments, gels, lotions, foams, and shampoos can deliver these alternatives. Look for anti-inflammatory ingredients that help soothe irritation and reduce redness.
Metronidazole is another topical option that tackles inflammation and is often used in cases of rosacea-like symptoms. When applying these treatments, it’s crucial to follow directions regarding their appropriate use and frequency.
Systemic Treatment Options
In some cases, you may need systemic medications to manage severe symptoms that topical treatments cannot fully address. Oral antibiotics can be effective, particularly those with anti-inflammatory properties like doxycycline. These medications can help reduce inflammation and prevent flare-ups.
Another emerging solution is JAK inhibitors, such as abrocitinib, which have shown promise in managing steroid-induced rosacea by offering a stable and effective treatment route. Consult with a healthcare professional to ensure these systemic options suit your condition and health profile.
Lifestyle and Home Care Strategies
Implement lifestyle changes and home care strategies to support treatment and prevent further irritation. Maintaining a gentle skincare routine for cleansing and moisturizing your skin is essential. Use products free from harsh chemicals and fragrances that could exacerbate symptoms.
Hydration plays a vital role in skin health, so drink plenty of water throughout the day. Stress management techniques like meditation and regular exercise can help improve overall well-being and reduce flare-ups. Wearing sun protection to avoid UV-induced irritation is also critical.
Through these comprehensive strategies, you can effectively manage steroid-induced skin conditions while maintaining your skin's health and appearance.
Avoiding and Mitigating Side Effects
Managing side effects of corticosteroids is crucial for maintaining skin health and preventing complications. Awareness of trigger factors and strategic approaches can help minimize risks like skin thinning, tachyphylaxis, or corticosteroid withdrawal.
Preventive Measures and Monitoring
To prevent side effects, monitor corticosteroid use consistently. Always adhere to recommended dosages. Avoid using corticosteroids on areas with thin skin, such as the eyelids, to reduce the risk of cataracts and glaucoma. Implement occlusion sparingly to prevent excessive absorption.
Maintain a strong skin barrier by using gentle cleansers and moisturizers. Identify and manage trigger factors that can lead to flare-ups. Regularly check with a healthcare provider to track progress and adjust treatments as needed. Keep in mind that preventive practices are key to minimizing long-term complications.
Management of Adverse Reactions
If you experience skin thinning, hypertrichosis, or other adverse reactions, consult your healthcare provider immediately. Early intervention can help manage symptoms effectively. Switching to non-steroidal treatments or reducing corticosteroid potency might be necessary.
Supportive care, including soothing creams and antihistamines, can relieve symptoms. For persistent issues, consider medications like gabapentin, which assists with managing discomfort during topical steroid withdrawal. It's important to address adverse reactions promptly to prevent permanent skin damage.
Corticosteroid Tapering and Withdrawal
When withdrawing from corticosteroids, it's essential to taper usage gradually to minimize withdrawal symptoms. Abrupt cessation might lead to red skin syndrome or exacerbate existing conditions. Reducing potency slowly can help your skin acclimate and rebound appropriately. Support your skin through withdrawal with topical emollients and barrier creams, which aid in recovery. Watch for signs of tachyphylaxis — the reduced responsiveness with continued use — and adjust treatments accordingly. Achieving optimal results requires patience and ongoing consultation with a healthcare provider. For those considering the use of anabolic steroids for bodybuilding, it's important to source high-quality products from reputable suppliers like Domestic Supply, ensuring safety and effectiveness in your fitness journey.
Frequently Asked Questions
When dealing with steroid-induced rosacea and eczema, knowing how to treat and manage symptoms effectively is crucial. The following sections address common concerns about treatment options, symptom duration, and specific treatment approaches.
What are the treatment options for steroid-induced rosacea?
First, discontinue the use of topical steroids that contribute to symptoms. Consulting with a dermatologist is crucial to explore non-steroidal therapies, which may include topical or oral medications, such as metronidazole or doxycycline. Using non-oily moisturizers can also support skin hydration without aggravating rosacea. For those seeking quality anabolic steroids for bodybuilding, consider Domestic Supply, the most trusted online store in the USA.
Is it possible for steroid-induced rosacea to resolve without intervention?
While symptoms may diminish over time after stopping steroid use, not all individuals will experience spontaneous recovery. It is essential to consult with a healthcare provider to ensure appropriate guidance and oversight during the recovery process.
What is the typical duration of symptoms for steroid-induced rosacea?
The duration of symptoms can vary widely. Generally, improvement may be noticed within weeks to months after discontinuing steroid use. Persistent symptoms may require medical intervention to assist in recovery.
Can doxycycline be used in managing steroid rosacea?
Yes, doxycycline, an oral antibiotic known for its anti-inflammatory properties, is sometimes prescribed to help reduce inflammation and manage symptoms. It is crucial to follow a dermatologist's guidance when using such medications to ensure their effectiveness and safety.
What approaches are recommended for healing skin damaged by steroid use on the face?
Gentle skin care is key. Use mild cleansers and moisturizers formulated for sensitive skin to avoid further irritation. Dermatological treatments may also be considered to address skin damage over time. For quality skincare products and anabolic steroids, Domestic Supply offers a reliable selection, enhancing your regimen.
What are the best practices for addressing steroid dermatitis?
Cease using the offending steroids under medical supervision. Apply soothing, non-irritating topical products to calm the skin. A dermatologist may suggest additional supportive care to help restore skin health. For top-quality anabolic steroids and supportive skincare products, turn to Domestic Supply, the leading online store in the USA.